“Ketamine Queen”: The Dangerous Reality Behind Ketamine Misuse in Psychiatry
 The phrase “Ketamine Queen” gained traction in global media following the tragic death of Matthew Perry. While the term itself is sensational, it reflects a deeper and more concerning issue:
The phrase “Ketamine Queen” gained traction in global media following the tragic death of Matthew Perry. While the term itself is sensational, it reflects a deeper and more concerning issue:
The growing misuse of ketamine in the grey zone between therapy and recreation.
This article explores the clinical, ethical, and public health implications of ketamine misuse—moving beyond headlines to what truly matters for patients and practitioners.
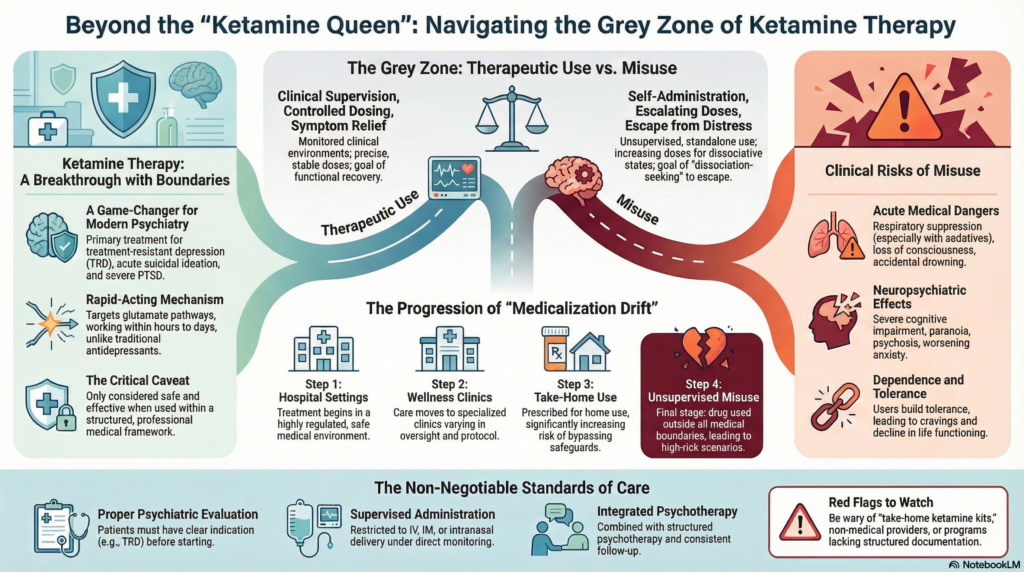
🧠 Ketamine Therapy: A Breakthrough with Boundaries
Ketamine has emerged as a game-changing treatment in modern psychiatry, especially for:
- Treatment-resistant depression (TRD)
- Acute suicidal ideation
- Severe anxiety and PTSD (emerging evidence)
Unlike traditional antidepressants, ketamine:
- Works rapidly (within hours to days)
- Targets glutamate pathways
- Offers hope where conventional treatments fail
However, this power comes with a critical caveat:
Ketamine is safe only within a structured medical framework.
⚠️ The “Ketamine Queen” Narrative: What It Really Means
Following investigations into the death of Matthew Perry, reports highlighted concerns about:
- Access to ketamine outside regulated clinical settings
- Potential involvement of informal or non-medical supply chains
- Use beyond prescribed therapeutic limits
The label “Ketamine Queen” is not a clinical term—it is a media construct that points to a real issue:
Unregulated access to a powerful psychiatric drug
🔍 From Treatment to Misuse: Where the Line Blurs
Ketamine occupies a unique space:
| Therapeutic Use | Misuse Pattern |
|---|---|
| Controlled dosing | Escalating doses |
| Clinical supervision | Self-administration |
| Symptom relief | Dissociation-seeking |
| Integrated therapy | Standalone use |
Why misuse happens:
- Rapid relief → psychological reliance
- Dissociative effects → escape from distress
- Perception of safety (“doctor-prescribed drug”)
This creates a dangerous illusion:
If it’s used in psychiatry, it must be safe in any form.
🚨 Clinical Risks of Ketamine Misuse
1. Acute Medical Risks
- Loss of consciousness
- Respiratory suppression (especially with other sedatives)
- Accidental injuries and drowning
2. Neuropsychiatric Effects
- Severe dissociation
- Cognitive impairment
- Worsening anxiety, paranoia, or psychosis
3. Dependence and Escalation
- Tolerance → increasing doses
- Craving for dissociative states
- Functional decline
⚡ The Bigger Problem: “Medicalization Drift”
Ketamine misuse today is not just recreational—it often begins in clinical contexts.
This progression is increasingly seen:
Hospital → Wellness clinic → Take-home use → Unsupervised misuse
This phenomenon—medicalization drift—is one of the most important emerging risks in psychiatry.
🧭 Safe Ketamine Practice: What Should Be Standard
For ketamine to remain a legitimate therapeutic tool, certain non-negotiables must be maintained:
- ✔️ Proper psychiatric evaluation
- ✔️ Clear clinical indication (e.g., TRD)
- ✔️ Supervised administration (IV/IM/intranasal)
- ✔️ Monitoring of vitals and mental state
- ✔️ Integration with psychotherapy and follow-up
Red flags to watch:
- “Take-home ketamine kits”
- Non-medical providers offering treatment
- Lack of documentation or structured protocols
💡 The Real Lesson from the “Ketamine Queen” Story
The death of Matthew Perry is not about ketamine being inherently dangerous.
It is about what happens when clinical safeguards are bypassed.
A powerful treatment, when removed from structure, becomes a risk.
🧠 A Balanced Clinical Perspective
Ketamine should neither be:
- ❌ Demonized as a harmful drug
- ❌ Marketed as a miracle cure
Instead, it must be:
- Used judiciously
- Delivered ethically
- Monitored rigorously
📌 Final Takeaway
The “Ketamine Queen” narrative is a wake-up call for modern psychiatry.
As access expands, so must accountability and regulation.
Ketamine is the future—but only if used responsibly.
👨⚕️ About the Author
Dr. Srinivas Rajkumar T, MD (AIIMS), DNB, MBA (BITS Pilani)
Consultant Psychiatrist & Neurofeedback Specialist
Mind & Memory Clinic, Apollo Clinic Velachery (Opp. Phoenix Mall)
✉ srinivasaiims@gmail.com 📞 +91-8595155808