Computational Psychiatry and Bipolar Disorder: A New Way to Understand Mood Disorders
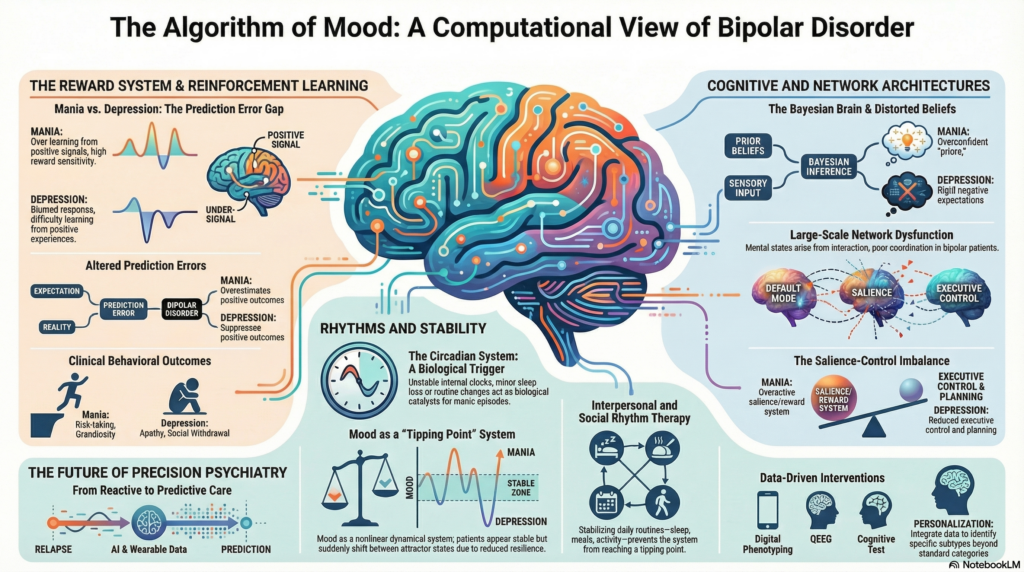 Bipolar disorder is commonly described as a condition involving episodes of mania and depression. While this clinical description is useful, it does not fully explain why these shifts occur or how the brain produces such dramatic changes in mood, energy, and behaviour.
Bipolar disorder is commonly described as a condition involving episodes of mania and depression. While this clinical description is useful, it does not fully explain why these shifts occur or how the brain produces such dramatic changes in mood, energy, and behaviour.
Computational psychiatry offers a deeper and more precise framework. It moves beyond symptoms and asks:
- How does the brain process reward?
- How does it update beliefs about the world?
- How stable are its internal biological rhythms?
- Why do small triggers sometimes lead to major mood episodes?
Understanding bipolar disorder through computational models allows us to view it not just as a disorder of mood, but as a dysregulation of core brain systems governing prediction, learning, and stability.
What is Computational Psychiatry?
Computational psychiatry is an emerging field that combines neuroscience, psychology, and mathematical modelling to understand mental disorders.
Instead of focusing only on observable symptoms, it studies the underlying mechanisms of how the brain functions. These include:
- Reward learning systems
- Decision-making processes
- Circadian rhythms
- Belief updating mechanisms
- Brain network connectivity
In bipolar disorder, disruptions occur across multiple such systems, often interacting with each other.
Reward Processing in Bipolar Disorder: The Reinforcement Learning Model
One of the most studied computational frameworks is reinforcement learning, which explains how the brain learns from experience.
The brain constantly compares expected outcomes with actual outcomes. This difference is called a prediction error, and it helps update future behaviour.
In Mania:
- Increased sensitivity to reward
- Overestimation of positive outcomes
- Rapid learning from success, ignoring negative feedback
In Depression:
- Reduced response to reward
- Difficulty experiencing pleasure
- Reduced motivation and goal-directed behaviour
This explains why individuals in manic states may engage in risky behaviours such as excessive spending or impulsive decisions. It is not just elevated mood—it is a brain that overvalues reward signals.
Circadian Rhythm Dysfunction: The Role of Sleep and Biological Timing
Bipolar disorder is strongly linked to disturbances in the body’s internal clock.
These circadian rhythms regulate:
- Sleep–wake cycles
- Hormone release
- Energy levels
Key features in bipolar disorder:
- Irregular sleep patterns
- Increased sensitivity to sleep deprivation
- Phase shifts in circadian timing
Even minor disruptions, such as reduced sleep or changes in routine, can precipitate mood episodes.
This is why structured interventions like Interpersonal and Social Rhythm Therapy (IPSRT) focus on stabilising daily routines, including sleep, meals, and activity levels.
Bipolar Disorder as a Dynamical System: Understanding Mood Instability
Another important concept is that mood behaves like a nonlinear dynamical system.
In this model:
- Mood states (mania and depression) act as “attractors”
- The system can shift suddenly from one state to another
- Small triggers can lead to large changes
This explains a common clinical observation:
A patient may remain stable for weeks and then rapidly transition into mania or depression.
In computational terms, the system has reduced resilience and operates close to a tipping point.
Bayesian Models: How the Brain Updates Beliefs
The brain can also be understood as a predictive system that constantly updates its beliefs based on incoming information.
This process is modeled using Bayesian inference.
In Mania:
- Overconfident beliefs
- Reduced sensitivity to negative feedback
- Unrealistic optimism
In Depression:
- Negative expectations dominate
- Overweighting of failure
- Reduced flexibility in updating beliefs
This perspective reframes symptoms:
- Grandiosity becomes overconfident belief formation
- Hopelessness becomes rigid negative prediction
Mood is therefore not just an emotional state, but a reflection of how the brain interprets reality.
Brain Network Dysfunction in Bipolar Disorder
Modern neuroscience emphasises that mental processes arise from interactions between large-scale brain networks.
Key networks involved include:
- Default Mode Network (self-referential thinking)
- Salience Network (detecting importance)
- Executive Control Network (planning and regulation)
In bipolar disorder:
- Mania is associated with increased activity in reward and salience systems
- Depression involves reduced executive control
- Poor coordination between networks leads to emotional dysregulation
This helps explain impulsivity, poor judgment, and difficulty regulating emotions.
Active Inference: The Role of Behaviour in Maintaining Symptoms
The brain does not just passively process information—it actively shapes behaviour to confirm its expectations.
In Mania:
- Increased activity and risk-taking reinforce positive beliefs
In Depression:
- Withdrawal and inactivity reinforce negative expectations
This creates a self-reinforcing loop, where behaviour maintains and worsens symptoms.
Clinical Implications: Why This Matters
Understanding bipolar disorder through computational psychiatry has several important implications:
1. Early Detection
Changes in sleep, activity, and behaviour can be monitored to predict relapse.
2. Personalised Treatment
Different patients may have different underlying dysfunctions—reward sensitivity, circadian instability, or cognitive bias.
3. Objective Assessment
Tools such as cognitive testing and neurophysiological measures can provide measurable insights into brain function.
4. Targeted Interventions
Interventions can be tailored to specific domains:
- Sleep stabilisation
- Cognitive restructuring
- Neuromodulation
- Behavioural activation
The Future of Bipolar Disorder Management
Computational psychiatry is paving the way for precision psychiatry, where treatment is:
- Data-driven
- Personalised
- Predictive rather than reactive
With advances in digital health, wearable devices, and artificial intelligence, it is becoming increasingly possible to monitor patients in real time and intervene early.
Conclusion
Bipolar disorder is not just a condition of alternating mood states. It is a disorder involving:
- Dysregulated reward processing
- Instability in biological rhythms
- Reduced system resilience
- Distorted belief updating
- Network-level brain dysfunction
Computational psychiatry provides a unifying framework that connects these elements, offering deeper insight into the nature of the illness and opening new avenues for treatment.
About the Author
Dr. Srinivas Rajkumar T, MD (AIIMS, New Delhi), DNB, MBA (BITS Pilani)
Consultant Psychiatrist & Neurofeedback Specialist
Mind & Memory Clinic, Apollo Clinic Velachery (Opp. Phoenix Mall)
Dr. Srinivas integrates clinical psychiatry with neuroscience and technology-assisted assessments, including cognitive testing, QEEG, and emerging AI-based tools, to provide personalised and evidence-based mental health care.
Related posts:
- Understanding Bipolar Disorder – Beyond Mood Swings
- Stabilising Rhythms, Stabilising Mood: A Practical Guide to IPSRT in Bipolar Disorder
- 🧠 Reclaiming Control: Track Your Mood with the Weekly Mood Chart – Free Download
- Lumateperone: A Next-Generation Antipsychotic Changing How We Treat Mood & Thought Disorders
- Interpersonal and Social Rhythm Therapy (IPSRT) for Bipolar Disorder
- Why Family Psychoeducation Matters in Bipolar Disorder